What is Scoliosis?
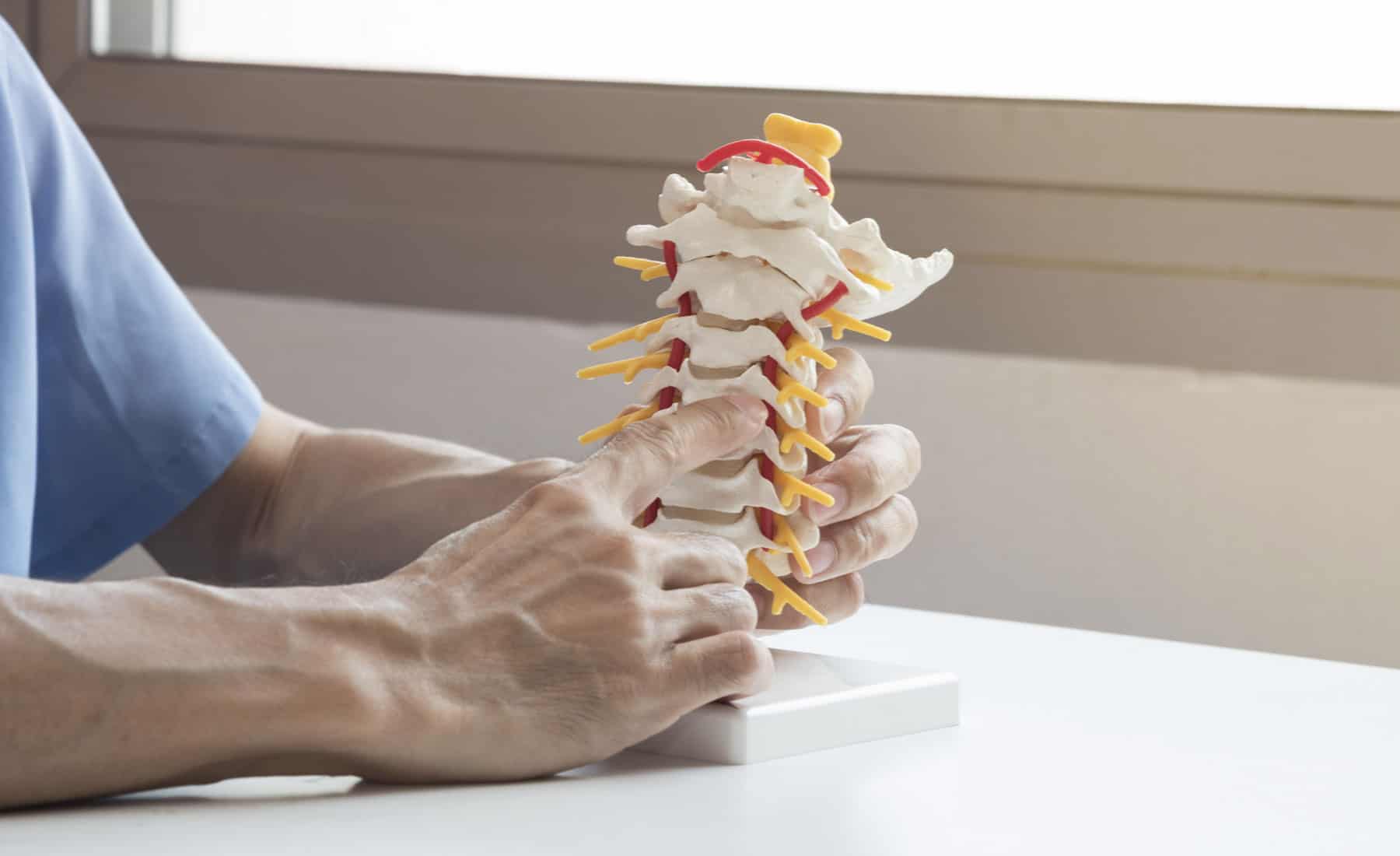
Scoliosis is a condition where the spine curves from side to side, rather than straight. This results in the spine having an “S” or a “C” shape when viewed from the front or back. People with scoliosis also frequently display some rotation of the spinal bones (or vertebrae) on each other, and some will also have a kyphosis (forward leaning of the spine).
Scoliosis can affect individuals at any age. In some cases there is a family tendency for this to occur, and the role of genetics is being increasingly understood. In children and adolescents with significant scoliosis, females are affected more often than males. Scoliosis can also occur in adulthood, particularly as the spine ages (degenerative scoliosis).
In most cases, the cause of scoliosis is unknown.
The main types of scoliosis are idiopathic scoliosis and adult degenerative scoliosis.
What is Idiopathic Scoliosis?
Idiopathic scoliosis develops in childhood. It can be divided into early onset idiopathic scoliosis, and late onset idiopathic scoliosis.
Early onset scoliosis occurs between birth and 9 years of age. Generally, the earlier the age of scoliosis onset, the more severe and disabling it may become. Early onset scoliosis can result in major lung problems due to lack of normal lung development, and sometimes can progress rapidly.
What is Adolescent Scoliosis?
Late onset scoliosis (also known as adolescent idiopathic scoliosis) typically has its onset between 10 to 18 years of age.
Adolescent Scoliosis is more common in females, and usually affects the thoracic (upper) spine and rib cage.
The lungs are usually developed by this stage and so lung problems are typically not as severe unless the scoliosis is quite major (over 80 degrees curve).
The greater the scoliosis, and the younger the individual, the higher the chance of curve progression.
If a child is under 14 years and seems to have a large amount of growth left, then they are likely to progress and therefore treatment will be recommended in most cases.
Bracing is usually recommended for 25 – 40 degree curves, with surgical treatment often advised if the curve increases to 50 degrees in a growing spine. Whilst this is classified as major surgery, most patients are able to return to normal activities by around 12 months postoperatively.
What is Adult Scoliosis?
There are two types of adult scoliosis:
- Adult Idiopathic Scoliosis. These patients have had scoliosis since childhood or adolescence. These people ‘bring the curve with them’ from childhood.
- Adult “De Novo” or Degenerative Scoliosis. This develops in adulthood. Degenerative scoliosis develops as a result of disc and facet joint degeneration. As the intervertebral discs degenerate, they lose height. If one side of the disc degenerates faster than the other side, the disc can tilt and this causes the spine to bend and curve.
Large curves more commonly result in back pain than smaller curves. Curves greater than 80 degrees in the thoracic spine may cause shortness of breath with activity, due to impairment of lung function.
While adult scoliosis rarely causes paralysis or other severe neurologic problems on its own, it can be associated with spinal stenosis (narrowing around the nerves) in the lumbar spine. This can result in nerve root compression or irritation, thereby causing leg pain, numbness and weakness.
Patients can also develop a kyphotic posture (the spine is bent forward) with the scoliosis, and also with age as the intervertebral discs degenerate.
Often the inability to stand up straight (the spine bending forward) is more of a problem then the side-side curve.
Does adult scoliosis progress?
Adult scoliosis can also progress with time. When curves reach 30 to 40 degrees, it is of some concern, but only some progress. Curves that reach 50 degrees tend to progress more rapidly.
What are the symptoms of scoliosis?
The most common symptom of scoliosis is the appearance of an abnormally curved spine. Initially, there are often only mild changes and may first be noticed by friends or family. The change in the curvature of the spine usually occurs very gradually, which is why it is often not picked up until it is obvious.
Routine screening for scoliosis of girls in the early years of high school is sometimes done, and many early cases are picked up in this way. Most often it is a family member or swimming teacher / sports trainer that sees an asymmetry in the spine.
Sometimes it will be picked up because one shoulder has “dropped” lower than the other. Other lower spinal curves have one hip to be higher than the other side, or the head to be a little off centre. A more prominent curve of one side of the rib cage can result from rotation of the thoracic vertebrae and the ribs. Clothes do not fit as they previously did- for example tops may not sit evenly, pant legs may appear longer on one side.
With more severe scoliosis, particularly when it involves the thoracic spine, it can be more difficult for the heart and lungs to work properly, resulting in shortness of breath and chest pain.
In most cases, childhood scoliosis is not painful, but in some cases back pain or leg pain can occur. There are other potential causes of back pain, which your doctor will need to exclude.
How is Scoliosis Diagnosed?
A clinical examination will usually allow the diagnosis of scoliosis, however X-rays are necessary to characterise it location and severity. A thorough scoliosis evaluation requires full length X-rays of the entire spine, now commonly undertaken using the EOS system. Magnetic resonance imaging (MRI) is also usually done, particularly if there is leg pain, numbness or weakness which may be due to nerve root or spinal cord compression, and to rule out other associated pathologies such as spinal cord tethering or syrinx.
How is Scoliosis Treated?
The treatment of scoliosis should be individualised. It is generally based on the specific symptoms and age of the patient, as well as their radiology.
Fortunately, not all patients with scoliosis require treatment – for example those without symptoms and who have minor curvatures which are not progressing, and those that are not likely to progress can be simply observed. Also, many scoliosis patients have very minor symptoms and live with their scoliosis without any specific treatment.
In general, larger curves in younger children are more likely to progress than smaller curves in more mature children and adolescents. Other factors may include curve location, age, and genetic factors, and any underlying cause.
Predicting the likelihood of curve progression is an important part of the decision making process in the management of scoliosis, particularly in children and adolescents. A number of factors appear to play an important role:
- Curve severity: larger curves are more likely to get worse with time
- Sex: females have a higher risk of progression than males
- Maturity: if the bones have stopped growing, the risk of curve progression is lower. Conversely, braces are most effective in children whose bones are still growing
- Curve location: curves in the thoracic spine deteriorate more often than those in the cervical or lumbar spine
Observation
In children and adolescents, traditionally many patients may have a “wait and see” observation period. This is often done when scoliosis is detected, but the curve is not large enough to recommend treatments such as bracing or surgery. Periodic monitoring of the progression of the curve is done by regular examination and radiological studies.
Bracing
Non-surgical treatment comprises bracing- where the individual wears an external brace for an extended period of time (typically 2-3 years) to try and stop the curve from getting worse. This is usually effective in the growing spine but does not have a role in adult scoliosis. Adjustable braces can be used to accommodate the growing spine. Wearing a brace doesn’t cure or reverse the scoliosis curve, however it usually prevents further curve progression.
Most braces are made of plastic and are customised to snugly fit the body. They are difficult to notice under the clothes, as they fit under the arms and around the ribs, lower back and hips. Braces are generally worn day and night, as their effectiveness increases with the number of hours a day they are worn. Children wearing braces usually can participate in most activities with a few restrictions. They can take off the brace for short periods to participate in sports if they wish. Braces are worn until the bones stop growing. This is usually around the time:
- Around two years after the onset of menstruation
- At the time when teenage boys need to shave daily
- When their height plateaus and they are no longer getting taller
Physiotherapy
Physiotherapy is sometimes recommended, however there is little evidence that this can make a long term difference to curve progression or the need for surgery. Physiotherapy can be helpful in treating pain of spinal origin, and patients with scoliosis and back pain would typically be treated with a course of physiotherapy to see whether this is of benefit to them.
Injections and Other Non-Surgical Interventional Pain Procedures
Patients with back pain and leg pain may receive some benefit from injection treatment to help relieve the leg pain. Radiofrequency denervations may also be of assistance.
These treatments are aimed at the pain, and do not change the shape of the spine.
Spinal Surgery
Scoliosis surgery involves correcting the spine shape and fusing it (stabilising) in it’s corrected position. Most commonly it involves the use of a variety of devices, including screws, hooks and rods, and sometimes wires. Surgery may be done from the back (this is most common) or the front of the spine, and sometimes a combination. The length of the fusion, in other words the number of spinal bones included, depends on the scoliosis type and also the area of the spine involved, and the surgical techniques used.
In the younger child, there are several surgical techniques for holding the spine straight, but still allowing control/maintaining spine growth as much as possible. These include growth rods, tethers, and magnetic rods.
In adult spinal deformity surgery, the shape of the spine is combined with the ‘wear and tear’ which as accumulated over the years. This makes the spine joints stiffer, and the patient is more likely to present with pain, either in the back itself, or as a result of compression on spinal cord or nerves.
Forward bending (kyphosis) is also more likely to be a problem as the spine wears. Therefore, the goal of adult spinal deformity (including scoliosis) surgery is to first remove pressure on the nerves, and second to improve the shape of the spine, and keep the spinal deformity from progressing further.
Potential complications of scoliosis surgery include bleeding, infection, spinal fluid leakage, pain, nerve damage and paralysis. Occasionally, the bone fails to fuse solidly and further surgery is needed.
Victorian Comprehensive Scoliosis Clinic
The Victorian Comprehensive Scoliosis Clinic at Precision Brain Spine and Pain Centre is a unique, highly specialised and multidisciplinary medical clinic dedicated to the assessment and customised treatment of individuals with spinal deformity, including scoliosis. We assess individuals of all ages, from young children to the elderly, and where surgery is required, this can be offered to patients aged 14 years and over (younger children will be referred to one of the children’s hospitals if surgery is thought to be necessary).
The Victorian Comprehensive Scoliosis Clinic is led by experienced spine and scoliosis surgeon Mr Greg Etherington. Mr Etherington has over 20 years of experience in the diagnosis and treatment of scoliosis, and works closely with other team members including our rehabilitation specialists, pain specialists, neurosurgeons, neurologists, physiotherapists and psychologists.
Patients referred to the Victorian Comprehensive Scoliosis Clinic will be assessed initially by two of our key team members:
- A pain specialist or rehabilitation medicine physician
- Clinic Director, Orthopaedic Spine and Scoliosis Surgeon Mr Greg Etherington
The aims of these two initial consultations include:
- Accurate diagnosis and detailed assessment of the scoliosis
- Assessment of the likely generators of pain and other symptoms
- Presentation of all on-surgical treatment options, including rehabilitation, injections and radiofrequency denervations, and bracing
- Estimation of the risk of curve progression
- Discussion of the surgical options where surgery is a likely recommendation
Following the initial consultations, and depending upon the outcome of the clinical assessment and radiological studies, patients may be given priority access to other team members including:
- Spinal physiotherapists
- Psychologists (including child and adolescent psychologists). Coping with a diagnosis of scoliosis is usually difficult for a child or adolescent, particularly if long term bracing or spinal surgery is being contemplated. In particular, teenagers are burdened not only with additional physical changes, but also extra emotional and social challenges on top of what they would ordinarily experience as part of growing up. Anger, insecurity, depression and fear are commonplace, and our team of psychologists are here to offer support and to help them navigate this difficult period
- Neurologists and neurophysiologists, particularly where nerve conduction studies are required
- Neurosurgeons, particularly where spinal cord tethering, syrinx, tumours, or Chiari malformations are diagnosed
To learn more about The Victorian Comprehensive Scoliosis Clinic and treatment for scoliosis, please contact us.